If you live in New Jersey, you have probably heard the “willpower” version of addiction advice at least once. It sounds like this: Just stop. Be stronger. Don’t hang around the wrong people. Think about your family. Families say it because they are scared, and people struggling say it to themselves because they want to believe the problem has a simple fix.
Here is the issue. Most people with addiction have already tried willpower in every form. They have made deals with themselves, promised “never again,” and meant it in that moment. They have gone days or weeks without using, then hit a wall when life gets loud again. Stress came back. Sleep fell apart. Anxiety spiked. Something painful happened. A craving landed like a punch, and the brain went straight to the fastest relief it remembers.
This is why evidence-based therapy matters. It does not treat addiction like a moral weakness. It treats addiction like a condition that changes thinking, emotions, and behavior patterns over time. Evidence-based care gives people tools that work on hard days, not just on motivated days. New Jersey programs built around proven methods, including Absolute Awakenings, often see the same thing: when a person stops trying to “out-muscle” addiction and starts using structured treatment, recovery becomes steadier and more realistic.
Objective
To explain why addiction in New Jersey cannot be solved by willpower alone, and to show how Evidence-Based Addiction Treatment in New Jersey works step by step, including clinical standards, therapy methods, relapse prevention, personalized planning, and dual diagnosis care.
Key Takeaways
- Addiction changes brain chemistry and stress response, which makes willpower unreliable during cravings.
- Evidence-based therapy teaches practical skills for triggers, emotions, and cravings, not just motivation.
- Treatment in New Jersey usually follows these stages: assessment, detox (if needed), level of care, therapy, and aftercare.
- Clinical standards at NJ rehab centers improve safety, consistency, and outcomes.
- Personalized plans and dual diagnosis care often make the difference between repeated relapse and long-term progress.
Why Willpower Sounds Right But Often Breaks Down
Willpower is appealing because it feels fair. If you choose the substance, you can choose to stop. The problem is that addiction does not stay in the “choice” category for long. Over time, the brain learns that the substance is the quickest path to relief, comfort, energy, calm, or escape. When the brain is under stress, it tends to chase the quickest solution it trusts.
That is why people often do well when life is calm and fall apart when life gets messy. A person can be sincere at 9 a.m. and relapse at 9 p.m. because the day brought exhaustion, conflict, loneliness, or panic. If you have ever tried to be patient when you are running on three hours of sleep, you already understand the basic concept. When the nervous system is overloaded, self-control drops.
Addiction adds another layer because the brain has a stored shortcut: “Use this, and the feeling changes fast.” That shortcut is not a character flaw. It is learned behavior reinforced by brain chemistry. Evidence-based therapy is built to interrupt that shortcut and replace it with something more stable.
How Addiction Changes The Brain And Behavior
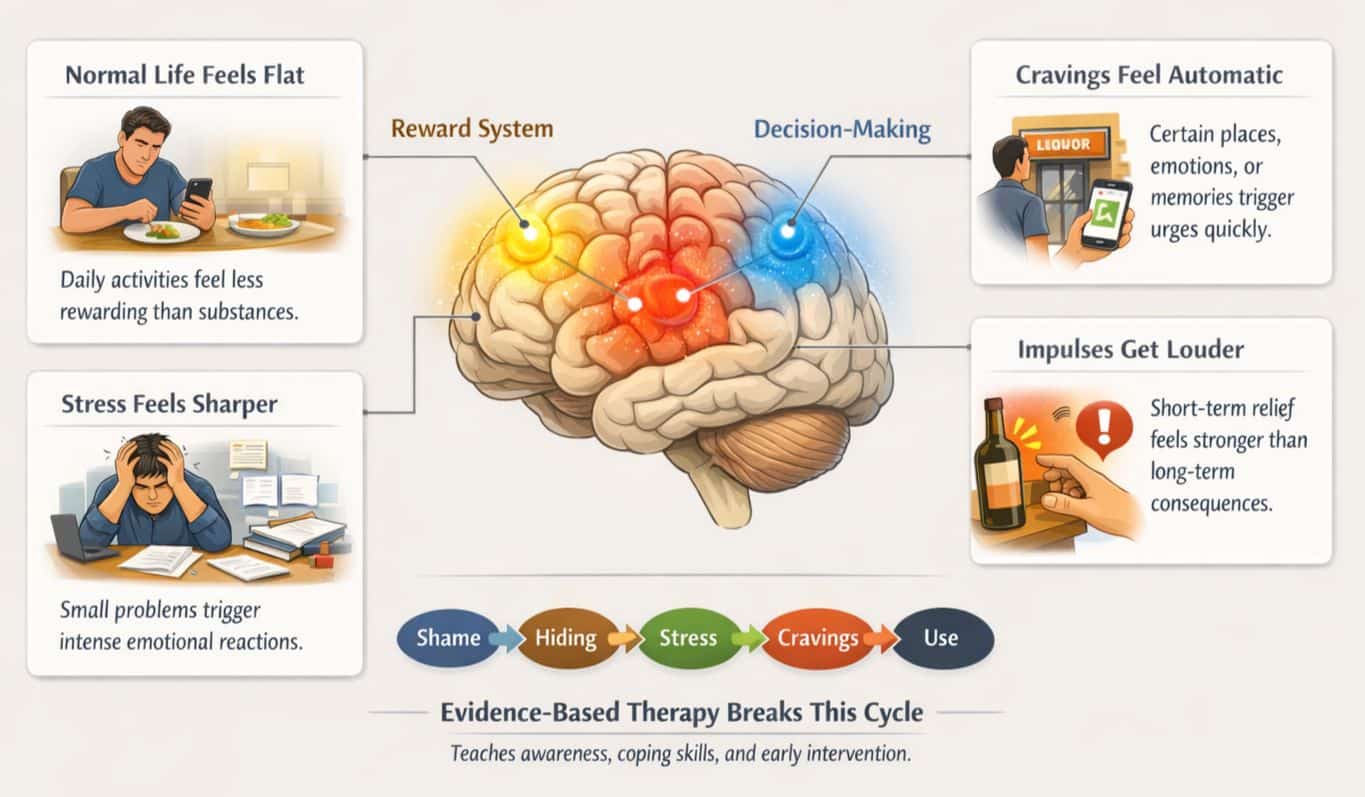
Addiction affects the brain’s reward system, stress system, and decision-making system. In simple terms, it changes what feels important, urgent, and tolerable.
Here are the changes many people notice as addiction grows:
- Normal life feels flat. Food, hobbies, and relationships feel less rewarding than they used to.
- Stress feels sharper. Small problems feel overwhelming, and emotions swing faster.
- Cravings feel automatic. A place, a payday, a certain friend, or a certain emotion can trigger a strong urge quickly.
- Impulses get louder. The brain pushes for short-term relief even when the person understands the long-term damage.
This is also why shame becomes such a problem. Shame makes people hide. Hiding increases stress. Stress triggers cravings. Then the cycle repeats.
Evidence-based therapy does not pretend that these patterns do not exist. It teaches people how to spot them early and respond differently before the urge becomes a full relapse.
What Evidence-Based Addiction Treatment In New Jersey Actually Means
Evidence-Based Addiction Treatment In New Jersey means treatment methods are chosen because they are proven to help, not because they sound inspiring or trendy. It also means progress is measured, plans are adjusted, and care is delivered by trained professionals following clinical guidelines.
In real life, evidence-based care focuses on practical questions like:
- What situations trigger cravings for you, specifically?
- What emotions do you avoid or numb with substances?
- What thoughts show up right before you use?
- What does relapse look like in your life, step by step?
- What coping skills will you use when the urge hits at 11 p.m. on a bad day?
That last part is important. A lot of “willpower” advice works only when a person feels calm and supported. Evidence-based therapy is designed for the moments when a person does not feel calm and supported.
The Key Stages Of Evidence-Based Addiction Treatment In NJ
Most New Jersey programs follow a sequence because recovery works better when it is built in layers. You stabilize first, then you build skills, then you plan for real life.
1. Assessment And Clear Diagnosis
This is not a quick intake and a generic plan. A proper assessment looks at substance use, physical health, mental health, home environment, and relapse history. It answers questions like: Is there a medical risk? Is there trauma? Is there anxiety or depression driving the cycle? What has worked before, and what has failed before?
A good plan starts with accuracy, not assumptions.
2. Medical Detox When Needed
Some people can stop without medical detox. Others cannot safely do that, or they cannot tolerate symptoms without relapsing. Detox is used when withdrawal is risky or intense, and it focuses on stabilization. That can include monitoring, symptom management, sleep support, hydration, and safety planning.
Detox is not the whole treatment. It is the floor you stand on, so therapy can actually work.
3. Inpatient Or Outpatient Levels Of Care
Not everyone needs the same structure. A person who has relapsed many times, lives in a high-trigger environment, or has serious mental health symptoms may need a more structured setting. Another person may do well in outpatient care with strong support and accountability.
The right level of care is the one that matches real risk, not pride.
4. Evidence-Based Therapy And Skills Practice
This is where change becomes real. People learn to recognize triggers, manage cravings, regulate emotions, and rebuild routines. Common evidence-based therapies include:
- CBT (Cognitive Behavioral Therapy): Helps people catch the thoughts that lead to use and replace them with healthier actions.
- DBT (Dialectical Behavior Therapy): Helps with emotional control, distress tolerance, and relationship conflict, which are major relapse triggers.
- Motivational Interviewing: Helps people strengthen their reasons for change without shame or pressure.
- Trauma-Informed Therapy: Helps people who use substances to cope with past pain or chronic fear.
This is also where programs like Absolute Awakenings often emphasize practice, not just talk. Skills work when you use them repeatedly, especially in the moments you would normally reach for a substance.
5. Aftercare And Relapse Prevention Planning
Aftercare is not an “extra.” It is the bridge between treatment and real life. This is where people build routines, support systems, and a plan for triggers. Aftercare can include therapy, group support, family work, and practical relapse prevention strategies.
If treatment ends with “good luck,” relapse becomes more likely. If treatment ends with a plan, recovery becomes more stable.
How NJ Rehab Centers Use Clinical Standards
Quality NJ rehab centers follow clinical standards because addiction treatment is medical and psychological care, not life coaching. Standards matter for safety, consistency, ethics, and outcomes.
Clinical standards often include:
- licensed clinicians and trained support staff
- medical protocols for detox when needed
- individualized treatment plans based on assessment
- regular progress reviews and plan adjustments
- confidentiality and ethical boundaries
- coordination for mental health needs and medications when appropriate
These standards reduce guesswork and risk. They also protect families from the chaos that often happens when addiction is handled informally and inconsistently.
How Evidence-Based Therapy Lowers Relapse Risk
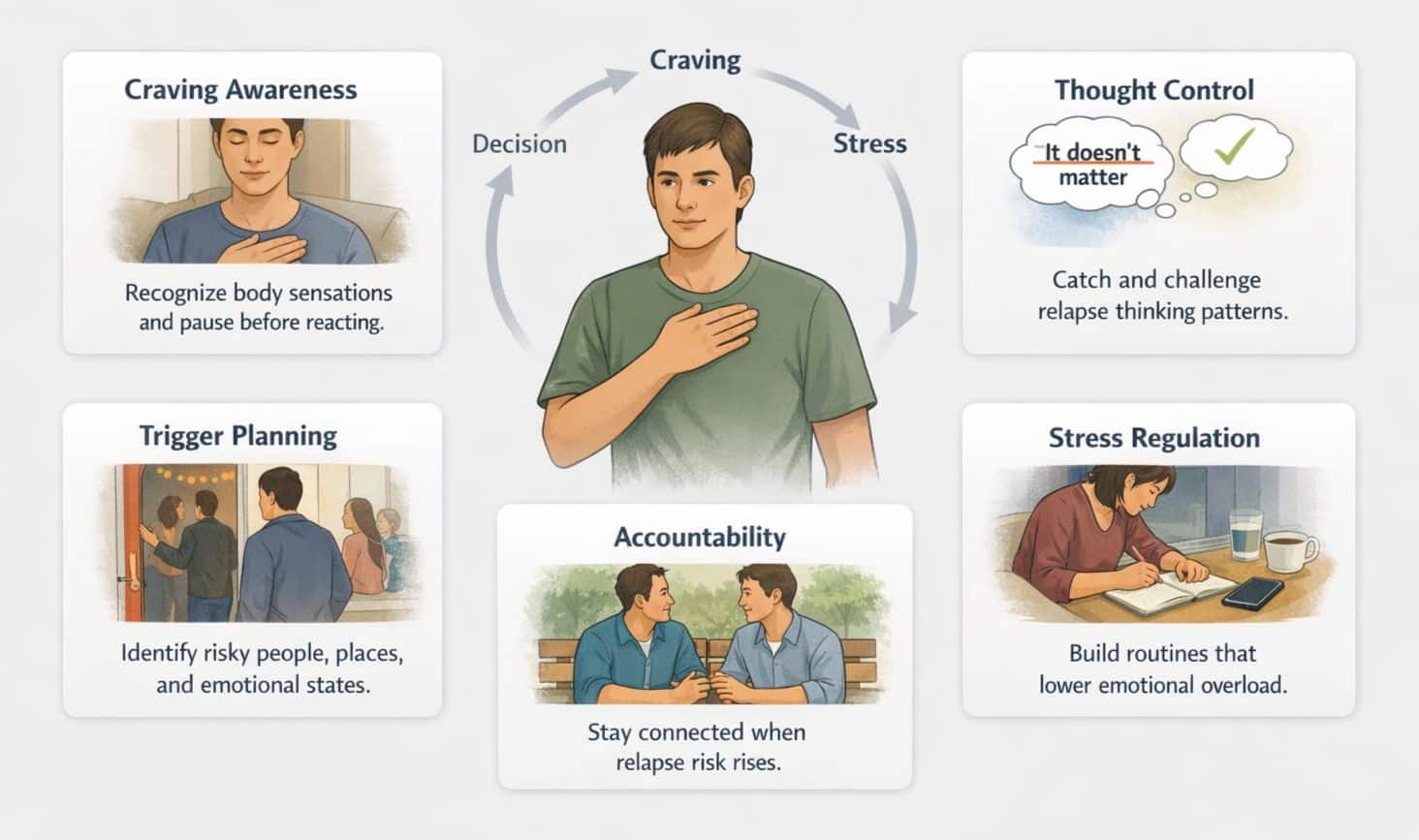
Relapse usually has a pattern. It rarely “just happens.” Evidence-based therapy helps people identify the pattern early and interrupt it.
Therapy often targets these areas:
- Craving Management: People learn what cravings feel like in their body and how to ride them out without panic.
- Trigger Planning: People identify the people, places, and emotions that lead to use and plan realistic boundaries.
- Thought Traps: People learn to catch thoughts like “I already messed up, so it doesn’t matter,” which often turns a slip into a spiral.
- Stress Skills: People practice coping methods that lower stress without substances, such as routines, sleep hygiene, and communication tools.
- Accountability: People build support so they are not alone at the exact moment they are most likely to relapse.
The goal is not to remove every craving forever. The goal is to help a person respond to cravings with skill instead of impulse.
Why Personalized Plans And Dual Diagnosis Care Matter
A major reason “willpower” fails is that it ignores the reasons a person uses it in the first place. Many people use substances to manage anxiety, depression, trauma symptoms, or chronic stress. If those issues remain untreated, the substance often returns because it still “solves” something, even if the solution is destructive.
Dual diagnosis care means treating addiction and mental health together. It is not two separate problems. For many people, it is one connected system.
Personalized treatment also matters because addiction looks different for different people. One person relapses after a conflict. Another relapse after loneliness. Another relapse after success because celebration triggers old habits. A good plan is built around the person’s real life, not a generic checklist.
Ready for Real Change in NJ?
If willpower hasn’t worked, structured evidence-based treatment in NJ can. Get personalized support that fits your real struggles.
A Simple Comparison Table
| Topic | Willpower-Only Approach | Evidence-Based Treatment Approach |
| Cravings | “Fight it” | Skills to manage urges and reduce intensity |
| Triggers | Avoid if possible | Identify, plan, practice responses |
| Stress | Push through | Emotional regulation and coping tools |
| Mental Health | Often ignored | Dual diagnosis support when needed |
| Relapse | Treated as failure | Treated as risk to reduce with planning |
Did You Know Facts
- Many relapses begin with sleep problems, isolation, and rising stress, not with a sudden “bad decision.”
- People are more likely to stay sober when they have a clear aftercare plan and consistent support.
- Treating anxiety, depression, or trauma alongside addiction often lowers relapse risk because the “need” for substances decreases.
- Skills-based therapy works best when practiced repeatedly, which is why structure matters early in recovery.
FAQs
1. Why Doesn’t Willpower Work For NJ Addiction?
Willpower matters, but addiction changes brain systems tied to reward and stress so that cravings can overpower intention, especially during emotional pressure. Evidence-based care builds skills and support that hold up when motivation drops.
2. What Is Evidence-Based Addiction Treatment In New Jersey?
It is a treatment that uses proven therapeutic methods, clinical standards, and structured stages of care, including assessment, detox (if needed), a level of care, therapy, and aftercare planning.
3. Do All People Need Medical Detox?
No, but many do, especially if withdrawal is risky, intense, or likely to cause relapse quickly. A professional assessment determines what is safest.
4. How Does Evidence-Based Therapy Reduce Relapse?
It teaches people to manage cravings, handle triggers, regulate emotions, and build relapse prevention plans. It replaces impulsive coping with practiced coping.
5. What Is Dual Diagnosis Care, And Why Is It Important?
Dual diagnosis care treats addiction and mental health together. It matters because untreated anxiety, depression, or trauma often fuels substance use and relapse.
Conclusion
It makes sense that people want a simple answer like willpower, because addiction is scary, and families want control. But the willpower story often leaves people feeling worse when they relapse, as if they proved they are weak or hopeless. That is not the truth. Addiction is a condition that reshapes behavior and brain chemistry over time, and recovery usually requires more than determination.
Evidence-Based Addiction Treatment in New Jersey offers something more practical: clinical care, proven therapy methods, structured stages of treatment, and long-term planning that supports real life. When care is personalized and mental health needs are addressed, people are not just “trying harder.” They are finally using tools that fit the problem. Programs like Absolute Awakenings reflect that approach by focusing on skill-building, stability, and a plan that lasts beyond the first burst of motivation.













